Whether it’s helping determine your service flow, choosing assessments and how they’re delivered, training clinicians or educating your service users—our team will guide your organization through a successful implementation and ensure that your Measurement Based Care project is successful and adapts to feedback along the way. Our support doesn’t stop at implementation or fit the traditional customer service model you’re used to; we are your partners and our team will be there to support you every step of the way.
The future of mental health care, now.
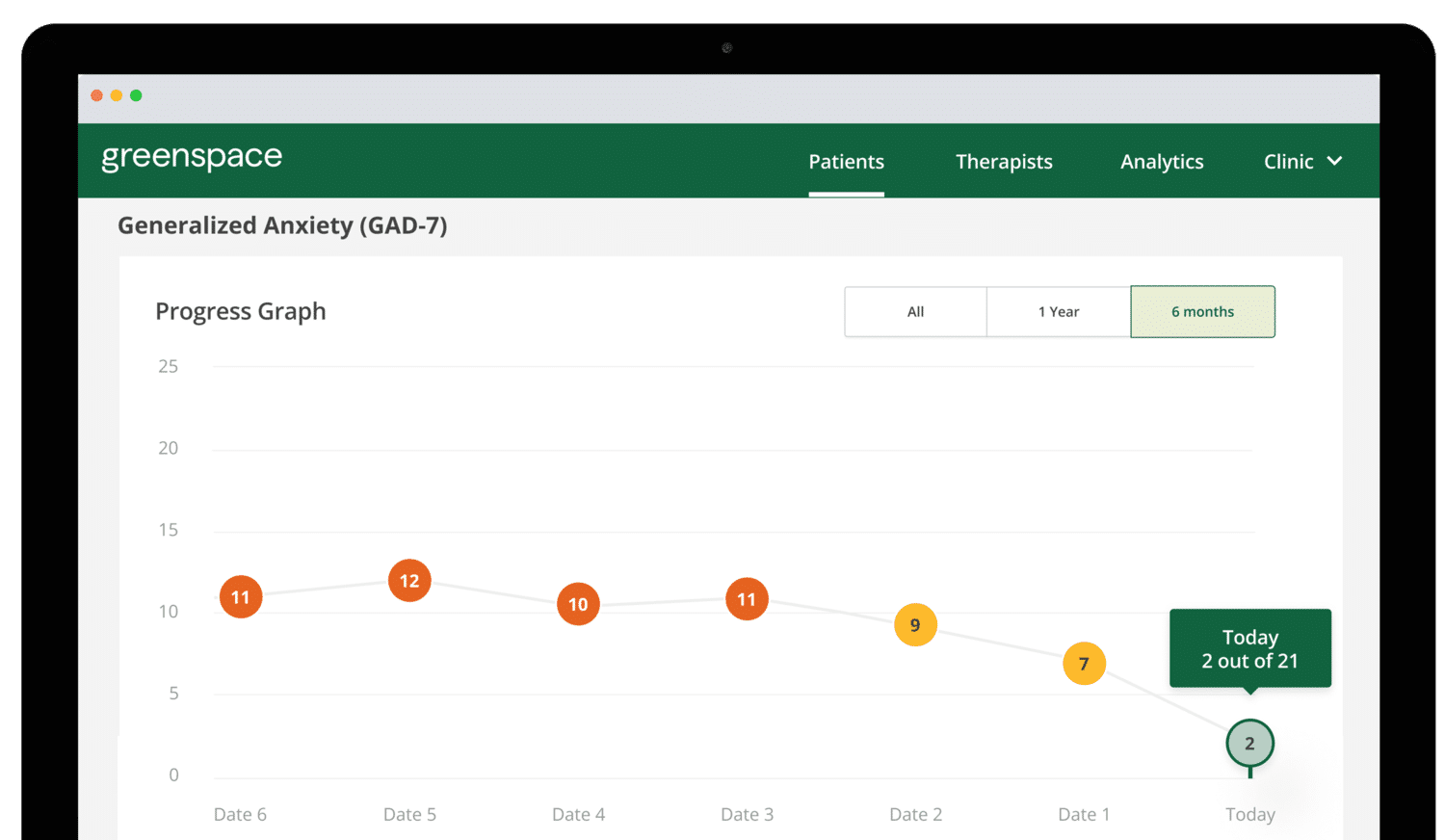
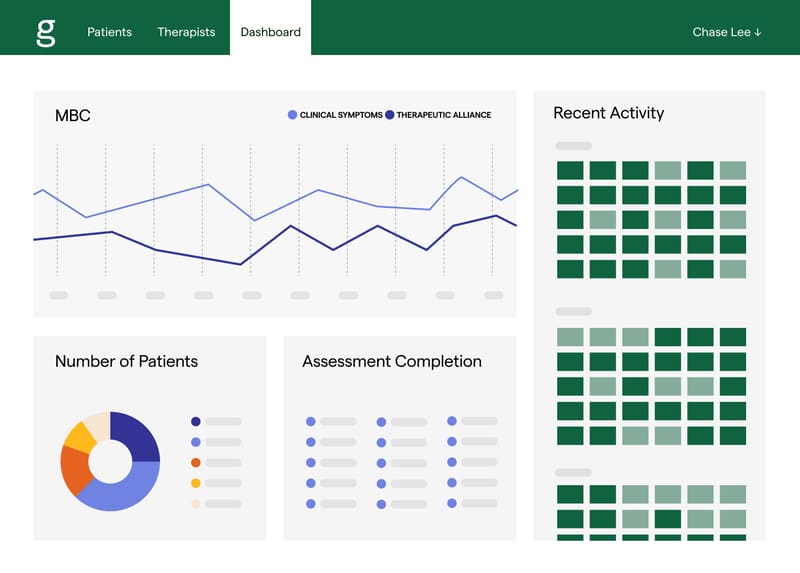
We’ve made Measurement-Based Care easier and more intuitive, so that you can focus on delivering the best possible care to the people you serve.
Learn More